My Third Trimester
Week 31
Estimated Reading Time: 9 minutes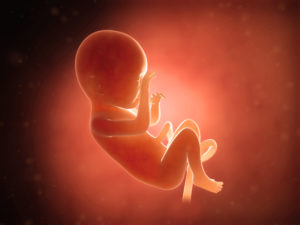 Arriving at week thirty-one, the central nervous system is now developed to the point where your baby’s body temperature is controlled by his or her brain. Your baby’s brain, body and systems are now working together and he or she is using all five senses and trillions of brain connections to grow. Little lungs are growing too but are not complete.
Arriving at week thirty-one, the central nervous system is now developed to the point where your baby’s body temperature is controlled by his or her brain. Your baby’s brain, body and systems are now working together and he or she is using all five senses and trillions of brain connections to grow. Little lungs are growing too but are not complete.
Your baby’s sexual development progresses; testicles are descending from the kidneys to the groin to the scrotum in boys. The labia continue developing but will cover the clitoris, which is observable in girls.
As opposed to sleeping, your baby is now enjoying more awake time and activity, which will probably be obvious to you. Your baby is now over 3 pounds and measuring 11 inches from crown to rump.
Preeclampsia
 One pregnancy complication affecting thousands of women and babies that has risen by twenty-five percent over the last twenty years is “Preeclampsia.” This serious medical problem affects 5%-8% of all pregnancies and 15% of these women develop HELLP (Hemolysis Elevated Liver enzymes and Low Platelets) Syndrome. Preeclampsia is a major source of maternal and infant illness and death. It usually occurs during the last half of pregnancy and rarely before Week 20; it may also strike in the postpartum period.
One pregnancy complication affecting thousands of women and babies that has risen by twenty-five percent over the last twenty years is “Preeclampsia.” This serious medical problem affects 5%-8% of all pregnancies and 15% of these women develop HELLP (Hemolysis Elevated Liver enzymes and Low Platelets) Syndrome. Preeclampsia is a major source of maternal and infant illness and death. It usually occurs during the last half of pregnancy and rarely before Week 20; it may also strike in the postpartum period.
You may be at risk for developing preeclampsia if any of the following apply to your Personal History:
- First pregnancy.
- Obesity (BMI>30).
- African-American or Caribbean descent.
- Over 35 or under 20 years of age.
- High blood pressure before becoming pregnant.
- High blood pressure or preeclampsia in previous pregnancies.
- Diabetes before or during pregnancy.
- Kidney disease.
- A mother or sister who had preeclampsia.
- Multiple gestations (e.g., twins, triplets).
- Rheumatoid arthritis, lupus or other autoimmune disorders
- Some blood clotting disorders.
- Polycystic ovarian syndrome.
- In vitro fertilization.
- Sickle cell disease.
Or your Family History:
- Preeclampsia.
- High blood pressure or heart disease.
- Diabetes
Early Onset Preeclampsia is defined as preeclampsia resulting in the delivery of your baby before Week 34; babies delivered earlier than expected may face lifelong disabilities. Early onset preeclampsia may result in sudden health complications for mothers and escalate their risk for long-term cardiovascular disease. Women who have had preeclampsia have roughly double the risk for heart disease and stroke over the next five to 15 years of their lives. Early onset preeclampsia contributes more to the morbidity and mortality of pregnant moms and their babies than preeclampsia acquired late in pregnancy.
Preeclampsia is typically hallmarked by an increase in blood pressure and signs of damage to another organ system, most often the liver or kidneys. A significant level of protein in the urine (proteinuria) is no longer a criterion for diagnosing preeclampsia, and may ultimately delay diagnosis and treatment. Preeclampsia may be diagnosed without proteinuria when there are signs of damage to other organs.
Symptoms of preeclampsia may include, but are not limited to:
- High blood pressure.
- Weight gain of more than 5 pounds in one week.
- Edema with swelling in the face, hands and feet.
- Nausea and vomiting.
- Headache.
- Blurred or altered visual disturbances.
- Chest pain or shortness of breath.
- Low back pain.
- Pain in the upper right abdomen area.
- Shoulder pain.
Remember that even a slight rise in your blood pressure may be a sign of preeclampsia. Women whose blood pressure had been normal or women who already have naturally high blood pressure may begin to see a change, usually after Week 20. Make sure you are evaluated at every visit to ensure that you are not exhibiting any signs or symptoms of preeclampsia. Call your health care team if you experience any symptoms of preeclampsia for the first time. If you are unable to reach them, go to the ER or the L&D to be evaluated by a health care provider.
“The earlier you know, the earlier you and your doctor can take steps to prevent or delay the onset of preeclampsia.”
HELLP syndrome is a life-threatening pregnancy condition and considered a severe variant of preeclampsia. Approximately 45,000 women will develop HELLP syndrome in the United States every year. The physical symptoms of HELLP syndrome may appear to be preeclampsia; it may sometimes be mistaken for the flu or gall bladder problems. It may include one or all of the following:
- Abdominal or chest pain and right upper quadrant pain (from liver swelling).
- Nausea/vomiting/indigestion with pain after eating.
- Headaches that won’t go away, even after taking medication such as Tylenol.
- Shoulder pain or pain when breathing deeply.
- Bleeding.
- Changes in Vision: blurred, seeing double or flashing lights.
- Swelling of the face or hands.
- Shortness of breath: breathing with difficulty, gasping.
The only cure for preeclampsia begins with the delivery of your baby. Your health care team will take many factors into account to manage your preeclampsia such as when to deliver, gestational age, the health of you and your baby and a careful evaluation of how the disease is progressing. Ultrasounds may be essential to monitor your baby’s growth and medications may be indicated for you. Hospitalization may also be required as your symptoms may unexpectedly worsen necessitating the need for the careful and precise monitoring of both you and your baby.
 Preeclampsia Foundations states: “When we urge women to trust themselves, we are referring to the intuitive feeling that preeclamptic women often have that “something is not right.” While these feelings may be nothing, it is important for women to report any concerns and for care providers to be diligent, particularly if accompanied by other signs or symptoms.”
Preeclampsia Foundations states: “When we urge women to trust themselves, we are referring to the intuitive feeling that preeclamptic women often have that “something is not right.” While these feelings may be nothing, it is important for women to report any concerns and for care providers to be diligent, particularly if accompanied by other signs or symptoms.”
If left untreated, preeclampsia can be dangerous and even fatal for both you and your baby. To ensure your and your baby’s wellbeing and to reduce bad outcomes from preeclampsia, it’s important to:
- Know the warning signs listed above.
- Trust yourself.
- Attend regular prenatal visits.
- Have a strong partnership with your health care team.
- If warning signs develop, call you health care team ASAP!
For further information regarding the signs, symptoms, care, treatment and how both preeclampsia and HELLP syndrome may affect you and your baby, please visit the Preeclampsia Foundation and the Mayo Clinic.
Preparing Your Baby’s “Safe to Sleep” Environment
 In a few short weeks you will be home and putting your baby down to sleep several times a day and throughout the night. Did you know the importance of making your baby’s sleeping environment a safe haven for sleep? According to a new policy statement by the American Academy of Pediatrics (AAP), “Infants should sleep in the same bedroom as their parents – but on a separate surface, such as a crib or bassinet, and never on a couch, armchair or soft surface — to decrease the risks of sleep-related deaths.” Babies should also “share their parents’ bedroom for at least the first six months and, optimally, for the first year of life, based on the latest evidence.”
In a few short weeks you will be home and putting your baby down to sleep several times a day and throughout the night. Did you know the importance of making your baby’s sleeping environment a safe haven for sleep? According to a new policy statement by the American Academy of Pediatrics (AAP), “Infants should sleep in the same bedroom as their parents – but on a separate surface, such as a crib or bassinet, and never on a couch, armchair or soft surface — to decrease the risks of sleep-related deaths.” Babies should also “share their parents’ bedroom for at least the first six months and, optimally, for the first year of life, based on the latest evidence.”
Sudden Unexpected Infant Death (SUID) or Sudden Unexpected Death in Infancy (SUDI) is a term used to describe any sudden and unexpected death, whether explained or unexplained occurring during infancy. Sudden Infant Death Syndrome (SIDS) is a subcategory of SUID and is a cause assigned to infant deaths that cannot be explained after a thorough case investigation.
It’s a fact that Sudden Infant Death Syndrome (SIDS) that was once cut by 50% is on the rise. It remains the leading cause of death among babies between one month and one year of age. So what can you do to insure you baby is safe when sleeping?
Become familiar with and follow the Safe to Sleep Guidelines recommended by the AAP, a proud partner in the national Back to Sleep Campaign that was spearheaded by the National Institute for Child and Human Development (NICHD).
Creating a safe to sleep environment for your expected baby is easy, logical and fun. There are nineteen guidelines listed in the AAP Policy Statement from November 2016; they are all equally important for you, your baby and everyone who takes care of your baby in any way. You’ll discover why you should place your baby on his or her back only, the problems that bed sharing can cause and the significance of implementing Tummy Time every day to name just a few!
The Recommendations To Reduce the Risk of SIDS and Other Sleep-Related Infant Deaths are:
- Back to sleep for every sleep.
- Use a firm sleep surface.
- Breastfeeding is recommended.
- It is recommended that infants sleep in the parents’ room, close to the parents’ bed, but on a separate surface designed for infants, ideally for the first year of life, but at least for the first 6 months.
- Keep soft objects and loose bedding away from the infant’s sleep area to reduce the risk of SIDS, suffocation, entrapment, and strangulation.
- Consider offering a pacifier at nap time and bedtime.
- Avoid smoke exposure during pregnancy and after birth.
- Avoid alcohol and illicit drug use during pregnancy and after birth.
- Avoid overheating and head covering in infants.
- Pregnant women should obtain regular prenatal care.
- Infants should be immunized in accordance with recommendations of the AAP and Centers for Disease Control and Prevention.
- Avoid the use of commercial devices that are inconsistent with safe sleep recommendations.
- Do not use home cardiorespiratory monitors as a strategy to reduce the risk of SIDS.
- Supervised, awake tummy time is recommended to facilitate development and to minimize development of positional plagiocephaly.
- There is no evidence to recommend swaddling as a strategy to reduce the risk of SIDS.
- Health care professionals, staff in newborn nurseries and NICUs, and childcare providers should endorse and model the SIDS risk-reduction recommendations from birth.
- Media and manufacturers should follow safe sleep guidelines in their messaging and advertising.
- Continue the “Safe to Sleep” campaign, focusing on ways to reduce the risk of all sleep-related infant deaths, including SIDS, suffocation, and other unintentional deaths. Pediatricians and other primary care providers should actively participate in this campaign.
- Continue research and surveillance on the risk factors, causes, and pathophysiologic mechanisms of SIDS and other sleep-related infant deaths, with the ultimate goal of eliminating these deaths altogether.
If you would like further clarification, please refer to SIDS and Other Sleep-Related Infant Deaths: Updated 2016 Recommendations for a Safe Infant Sleeping Environment.
For more information on Safe to Sleep, visit the AAP, NICHD and the CDC.