My Third Trimester
Week 29
Estimated Reading Time: 6 minutes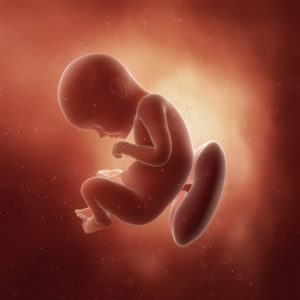 Your baby’s bones have completely matured at this gestational marker, although they remain supple. Baby is gearing up for an increase surge in growth. Weighing in at nearly 3 pounds and a little over 10 inches in length, your baby’s actions are now robust, even making you gasp at times! Your baby may be just about 3 inches away from his or her delivery day length but still needs to gain some more weight. By the time delivery day is here, your baby will have at least doubled or nearly tripled this week’s weight.
Your baby’s bones have completely matured at this gestational marker, although they remain supple. Baby is gearing up for an increase surge in growth. Weighing in at nearly 3 pounds and a little over 10 inches in length, your baby’s actions are now robust, even making you gasp at times! Your baby may be just about 3 inches away from his or her delivery day length but still needs to gain some more weight. By the time delivery day is here, your baby will have at least doubled or nearly tripled this week’s weight.
Nuchal Cords
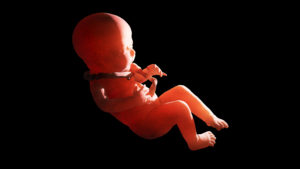 Through scientific research, we know that umbilical cord abnormalities are seen in one-third of all live births. Cerebral palsy and quadriplegic cerebral palsy are a direct result of such umbilical cord abnormalities.
Through scientific research, we know that umbilical cord abnormalities are seen in one-third of all live births. Cerebral palsy and quadriplegic cerebral palsy are a direct result of such umbilical cord abnormalities.
There are two types of nuchal cords; A & B. Type A encircles the neck in an unlocked pattern. Type B encircles the neck in a locked pattern, and this second type is responsible for 1 in 50 stillbirths according to Dr. Collins.
Nuchal cords are extremely common and most babies can wriggle their way out of them prior to settling into the head down position. Still, all nuchal cords have the potential to be extremely problematic. Dr. Collins also stresses that the problem may not be where the cord is or how it may be tangled but how much “slack” (defined as not tight or stretched taut, but hanging loosely or having a good deal of give) the baby has in the cord. For instance, in a tight cord with little slack, blood flow may be compromised through the cord. In this case, a nuchal cord can become a serious condition. The amount of cord slack can be assessed during Cord Doppler tests. A baby can have a nuchal cord during the entire pregnancy, up until delivery, but the cord needs to remain slack. The most important aspect of dealing with any type of umbilical cord concern is to be aware of its presence, so if the baby starts having changes in patterns of movement and heart decelerations when monitored, you may know now that a cord issue may be the cause.
If your baby does not wriggle out of his or her nuchal cord and it remains, discuss with your health care team the need for closer monitoring solutions such as frequent office visits, ultrasounds (ultrasounds are the only way your baby’s umbilical cord can be seen in utero), BPP, NST, Cord Doppler tests to show blood flow, very diligent movement counting and daily home fetal heart rate monitoring.
Fetal Non-stress Test (NST), Biophysical Profile (BPP) and Cord Blood Flow Doppler Test
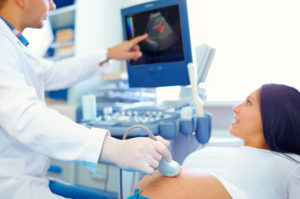 Three tests to check on your baby’s well-being in utero are a NST, a BPP, and a Doppler Ultrasound. The first test, an NST, will monitor and evaluate your baby’s heartbeat. This test usually starts in the third trimester (for high risk moms as early as the Week 28) for moms and expected babies who need special care and monitoring with conditions such as diabetes or hypertension, blood clotting disorders, follow up for an amniocentesis, IUGR, a baby who is small or not growing properly, a less active baby, if you have passed your due date or if you have had a previous loss. A NST usually takes 20-40 minutes to complete. Your baby’s heartbeat will be heard and recorded while your baby is inactive and active. The NST is a reactive test meaning your baby’s heart beats faster when moving. To be reactive, this must happen at least two times in 20 minutes. If your baby is sleeping or inactive, you may be given juice or water to drink to encourage your baby to move (although there is no scientific research to support this theory.) The NST will be considered nonreactive if your baby’s heart does not beat faster when your baby is active, or quiet and not moving. Don’t panic if this happens! They will consider this a false NST, but it merely means the NST did not provide enough information and additional tests such as a BPP may be necessary.
Three tests to check on your baby’s well-being in utero are a NST, a BPP, and a Doppler Ultrasound. The first test, an NST, will monitor and evaluate your baby’s heartbeat. This test usually starts in the third trimester (for high risk moms as early as the Week 28) for moms and expected babies who need special care and monitoring with conditions such as diabetes or hypertension, blood clotting disorders, follow up for an amniocentesis, IUGR, a baby who is small or not growing properly, a less active baby, if you have passed your due date or if you have had a previous loss. A NST usually takes 20-40 minutes to complete. Your baby’s heartbeat will be heard and recorded while your baby is inactive and active. The NST is a reactive test meaning your baby’s heart beats faster when moving. To be reactive, this must happen at least two times in 20 minutes. If your baby is sleeping or inactive, you may be given juice or water to drink to encourage your baby to move (although there is no scientific research to support this theory.) The NST will be considered nonreactive if your baby’s heart does not beat faster when your baby is active, or quiet and not moving. Don’t panic if this happens! They will consider this a false NST, but it merely means the NST did not provide enough information and additional tests such as a BPP may be necessary.
A BPP combines both fetal heart rate monitoring (NST) and a fetal ultrasound. Your baby’s breathing, heart rate, movements, muscle tone and amniotic fluid level are calculated and scored. The ideal goal is to get 10 out of 10. This simple combination of testing does not cause any physical danger to you or your baby. A BPP is normally performed as early as the 28th to 32nd week of pregnancy. It may, however, be considered when your doctor is planning an early delivery, typically after the 24th to 26th week of your pregnancy. A low score on a biophysical profile might indicate that you and your baby need further monitoring or special care. In some cases, early or immediate delivery might be necessary.
A Doppler Ultrasound checks the blood flow within the umbilical cord. A healthy umbilical cord will have two arteries, one vein, be the proper length and contain adequate Wharton’s Jelly. Wharton’s Jelly is a specialized tissue which serves many purposes for the developing fetus. Its specialized cells contain gelatin-like mucus that encase fibers. These properties give it an elastic and cushiony effect, which can tolerate the vibration, bending, stretching and twisting of an active fetus. In addition, it holds the vessels together, may regulate blood flow, plays a role in providing nutrition to the fetus, stores chemistry for the onset of labor, and protects the supply line. The Doppler Ultrasound may be more pivotal for umbilical cords that have only one artery, but it can also alert your health care team to other umbilical cord issues such as a knot, a kink, twisting or torsion, a nuchal cord and a short or long cord. This simple procedure tests the velocity and direction of the blood flow.
 If you’ve had a previous stillbirth due to a UCA, your health care team can assign a perinatologist or maternal fetal specialist who can schedule a NST and BPP anywhere from one to three times a week depending on moms comfort level to monitor the health of her baby. Remember that if you’ve had a pervious loss or complication, your doctor should absolutely label your next pregnancy as high risk!
If you’ve had a previous stillbirth due to a UCA, your health care team can assign a perinatologist or maternal fetal specialist who can schedule a NST and BPP anywhere from one to three times a week depending on moms comfort level to monitor the health of her baby. Remember that if you’ve had a pervious loss or complication, your doctor should absolutely label your next pregnancy as high risk!
In the presence of a nuchal cord, movement counting is especially important now and for the duration of your pregnancy if the nuchal cord remains or if your health care team considers the cord tight with or without kinks. Remember, changes in your baby’s movements, such as speeding up or slowing down, or changes in sleep-wake cycles could be a sign that your baby is not well. Dr. Collins advocates an ultrasound be done if decreased fetal movements are noted for a day. Know when your baby is awake and when he or she is asleep. Becoming your expected baby’s guardian through awareness, a proactive attitude and vigilance will empower you.