My Third Trimester
Week 28
Estimated Reading Time: 7 minutes Welcome to the third and last trimester of your pregnancy. By now you are anxious to meet your little baby. You are twenty-eight weeks into your pregnancy, whereby your baby has a 90 percent chance of being delivered healthy at this time. As every week passes, your baby’s likelihood of enjoying a healthy delivery day is enhanced.
Welcome to the third and last trimester of your pregnancy. By now you are anxious to meet your little baby. You are twenty-eight weeks into your pregnancy, whereby your baby has a 90 percent chance of being delivered healthy at this time. As every week passes, your baby’s likelihood of enjoying a healthy delivery day is enhanced.
Your little one’s brain continues to mature and increase in size. Your baby’s eyelids, surrounded by eyelashes, are somewhat open. Brief naps from 20–30 minutes will be taken. Wrinkles are decreasing on your baby’s skin as weight is increasing. Your baby is nearly 10 inches long, the length of a long slender cucumber, and weighs nearly 2¼ pounds.
Your Baby’s 28-Week Ultrasound
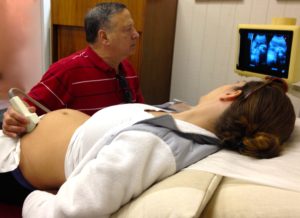 Request an ultrasound around this time to examine the umbilical cord and placenta for normal development and position. Request that EPV be measured at this and every ultrasound (visit Week 7 to learn the importance of keeping up-to-date with placental measurements.)
Request an ultrasound around this time to examine the umbilical cord and placenta for normal development and position. Request that EPV be measured at this and every ultrasound (visit Week 7 to learn the importance of keeping up-to-date with placental measurements.)
According to Dr. Collins, who has been researching Umbilical Cord Accidents (UCA) for over 25 years, it is typically during Weeks 28–30 when a problem could arise with your baby’s umbilical cord. He also believes an ultrasound at this time could detect a potential problem, making it a useful tool. The umbilical cord is a definite risk factor during the later part of your pregnancy and could compromise your baby.
Both Drs. Kliman and Uma Reddy, MD, MPH, Medical Officer Pregnancy & Perinatology Branch, Eunice Shriver National Institute of Child and Human Development, concur that UCAs, including nuchal cords, true knots, twists, torsion, kinks and long or short cords, account for 16 percent of the 26,000 yearly deaths in utero in the USA. That is at least 71 untimely deaths each and every day in our country. Dr. Collins states a UCA is not a “rare condition or event” and should be watched for especially in the last trimester of pregnancy. He advocates an ultrasound be done if decreased fetal movements are noted for a day.
After your ultrasound
If a problem is seen on your baby’s ultrasound with the umbilical cord or placenta, a plan of action needs to be decided upon with your health care team. Examples of close monitoring include repeat office visits, ultrasounds, Fetal Non-Stress Tests (NST), Biophysical Profiles (BPP), Cord (blood flow) Doppler tests, very diligent movement counting and daily home fetal heart rate monitoring.
If you and your health care team determine your baby should have further monitoring following your 28 week ultrasound, or you are considered high risk, don’t panic! It is comforting and reassuring to know your baby is healthy and stable thanks to the frequent monitoring. The four main reasons for monitoring your baby are to ensure that your baby is comfortable in utero, to ensure that your baby’s heart rate is normal and steady with no significant decelerations (decels) present, the placenta is working efficiently and not appearing to be aged, and to ensure that there are no signs of preterm or premature labor present.
“Most women who notice a decrease in movement will still have a healthy outcome,” says Obstetrician-Gynecologist Ruth Fretts, M.D., MPH, Assistant Professor at Harvard Medical School and Chair of the Stillbirth Review Committee at the Brigham and Women’s Hospital in Boston. “The biggest concern is when it happens repeatedly.” Dr. Fretts reminds every mom that as her pregnancy advances and her expected baby has less space, the kicks (movements) won’t be as strong and obvious. But if it takes you more than two hours to count 10 kicks (movements), your health care team should be called. She says a Non Fetal Stress Test (NST) is necessary to confirm your baby’s heart rate, “This rules out a life-threatening emergency, but it doesn’t address the underlying reason for decreased movement.”
Dr. Fretts says an ultrasound may add additional clarification. Unfortunately in the United States ultrasounds will be performed only about 20% of the time in these situations, so mom will need to assert her proactive skillfulness requesting one is done. With a normal NST, movement counting should be completed and charted every day. Mom should never hesitate to be evaluated every time a problem is perceived.
If the thought of counting and charting your baby’s movements makes you nervous, remember that movement counting is the safest and easiest course of action that every mom can take to monitor her baby’s movements on a daily basis. This simple concept is also free and non-invasive. Studies inform us that being attentive to your baby’s movements and informing your health care team of any changes such as speeding up or slowing down, or changes in sleep-wake cycles will decrease the likelihood of having a stillbirth. Ask your health care team about the signs of a baby that is not well and their protocol for such signs.
Movement Counting
 Since prenatal appointments are not on a daily basis, it is up to you to pay close attention each day to your baby’s movements. By simply counting your baby’s movements, this non-invasive, easy, and free method allows you to get to know your baby’s movement patterns and will alert you to the possibility of a potential problem.
Since prenatal appointments are not on a daily basis, it is up to you to pay close attention each day to your baby’s movements. By simply counting your baby’s movements, this non-invasive, easy, and free method allows you to get to know your baby’s movement patterns and will alert you to the possibility of a potential problem.
Mama, Can You Feel Me? Movement Counting Directions:
Beginning at Week 28, it’s time to feel, count and track your baby’s daily movement patterns! Find a comfy position and…
- FEEL your baby’s movements! Every kick, nudge, jab, flip, punch, roll, or twirl (not hiccups) counts.
- COUNT your baby’s movements! Once daily, time how long it takes for 10 movements in 1 hour (max 2 hours).
- TRACK your baby’s movements! Use our FREE app, ME Preg, or our paper tracking chart.
If you notice any changes in your baby’s movement patterns, such as a decrease, increase, or absence in fetal movement, CALL your health care team immediately to make sure that your baby is well. If you are unable to reach or visit your health care team, go to Labor and Delivery or the Emergency Room. Do not wait until the next day or next appointment!
You know your baby best, so always trust your instincts.
PAK’s Movement Counting Philosophy
 We strive for each expected baby to grow and develop in the best possible way, and ideally, to complete 40 weeks of nesting in utero healthy, strong, and ready to come into the world. A healthy delivery is our target. And on delivery day, don’t all babies deserve the best chance to arrive alive and kicking? If you have not been using our mobile app ME Preg, start now! ME Preg will help you to manage your pregnancy right up to delivery day. You can check off third trimester highlights, capture daily bump photos, schedule your important third trimester appointments, browse the latest pregnancy info, meditate and most importantly beginning at Week 28, track your baby’s daily movements.
We strive for each expected baby to grow and develop in the best possible way, and ideally, to complete 40 weeks of nesting in utero healthy, strong, and ready to come into the world. A healthy delivery is our target. And on delivery day, don’t all babies deserve the best chance to arrive alive and kicking? If you have not been using our mobile app ME Preg, start now! ME Preg will help you to manage your pregnancy right up to delivery day. You can check off third trimester highlights, capture daily bump photos, schedule your important third trimester appointments, browse the latest pregnancy info, meditate and most importantly beginning at Week 28, track your baby’s daily movements.
If you do not have a smartphone, begin using our MOM & BABY TRACKING CHART now! Let us help you journal this special time for both you and your baby. By recording your own personal pregnancy milestones in our MOM & BABY TRACKING CHART, together with your baby’s, you can also monitor and track your baby’s daily movements from one health care visit to the next.
Vaccinations During Pregnancy
If you are not current with your vaccinations, you have discussed being vaccinated with your health care team and you would like to be vaccinated, Dr. McGregor advocates being immunized around this gestational marker for Influenza (Inactivated) and Tdap (Tetanus, Diphtheria and Pertussis). The Tdap vaccination is also recommended for relatives, friends and caregivers who will spend time with your baby.

Photo by Suhyeon Choi on Unsplash